|
A preview of the papers appearing in the June 2007 issue of the Journal of the SID. To obtain access to these articles on-line, please go to www.sid.org
Edited by Aris Silzars
Medical displays in the healthcare system
Adi Abileah
Planar Systems
Abstract — As the healthcare system changes and progresses, the need for different types of high-performing displays is also evolving. There are three categories of displays: (a) embedded (as part of life-saving devices), (b) informative (for patient data and history, and managing workflow), and (c) imaging (high performing for diagnosis). The challenges of AMLCDs, which are the display of choice at the moment mainly in digital imaging, will be discussed. These challenges include very high resolution, high brightness, and wide viewing angle. The current performance of AMLCDs and the areas which they need to improve will be reviewed. A brief summary of the standards used to specify medical (diagnostic) displays will follow. A look into the future will predict the role of displays in hospitals.
Digital imaging (DI) is a more-demanding area of the healthcare system. Based on the imaging device and viewing the results on the display, a critical diagnosis is made. In many instances it can be a question of life or death. Therefore, the responsibility of the display specifications and performance are very important. In the case of X-ray imaging, the quality of the X-ray sensors, electronics, and the display, all as a system, has to match or exceed the performance of X-ray films. This is not trivial. Therefore, very-high-resolution displays need to be used.
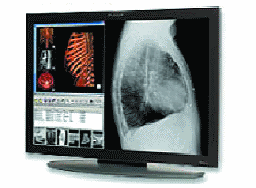
FIGURE 8 — A 4-Mpixel display showing typical information.
Image display in endoscopic surgery
Christopher S. Muratore
Beth A. Ryder
Francois I. Luks
Brown Medical School
Abstract — Advances in the technology of optical displays have changed the way surgeons are able to manage different illnesses. Minimally invasive surgery encompasses a wide range of endoscopic procedures, whereby the body cavity (abdomen, thorax, gastrointestinal tract, and joint spaces) is accessed through small incisions and the use of telescopes and fine, long instruments. These techniques have rapidly gained in popularity during the last decades, as patients are experiencing less discomfort after surgery. Visualization of the operative field requires optimal image capture, processing, and display. The introduction of charge-coupled devices has enabled surgeons to view the operative field on a video monitor, allowing ever-more-complex operations to be performed endoscopically. However, limitations include loss of 3-D perception and tactile sense, poor ergonomics, often suboptimal positioning of the image display, and image quality that is too dependent on outside influences. These limitations, and possible solutions, are addressed as is the "ideal" display system for endoscopic surgery.
Recently, flat-panel liquid-crystal-display (LCD) monitors have provided an improved image quality at a reduced price, and many operating rooms are now replacing CRT monitors with flat screens. Their light weight, versatility, and small footprint allow the use of multiple screens placed near the operating table. While LCD monitors produce the best image and have a greater portability than CRT monitors, the positioning of the screen is still limited by a number of factors, including the need to keep the immediate surroundings of the operative field sterile and the presence of a large number of instruments, instrument tables, cables, and other equipment that add to the clutter of the endoscopic operating room (Fig. 4).
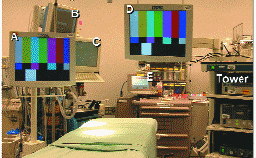
FIGURE 4 — Typical laparoscopic operating room set-up. Note the multitude of image displays: Two flat-screen laparoscopic monitors (A and D, off the laparoscopic "tower"), vital signs and anesthesia parameters display (B), patient data entry and display system (C), and drug-information display (E).
Improving information quality of MR brain images by fully automatic and robust image analysis methods
Ahmet Ekin
Radu Jasinschi
Jeroen van der Grond
Mark van Buchem
Philips Research
Abstract — The medical experts are expected to make diagnosis on an ever-increasing amount of data. Although the intention with the technological advances in imaging devices, such as MRI (magnetic resonance imaging), is to improve the medical practice, the increased amount of data may make the medical expert's task even harder and could arguably be counter-productive. A more desirable situation for the medical expert is the improvement in the clinical relevance of the image content and a faster, preferably automated, access to the most relevant part of the existing large amount of data. To this effect, the concept of information quality is introduced, and fully automatic, fast, and robust image analysis methods that improve it are proposed. As a guideline for a general framework, these methods are classified by the type of information they can improve: geometric, structural (sub-organ), and organizational. The algorithmic contributions are in the domain of MR brain image analysis. These methods improve the information quality not only for the visualization and the diagnosis by the expert, but also for the quantification by other automated methods. The robustness of these algorithms has been extensively tested at the Leiden University Medical Center over a large database of 550 patients.
The geometry of the brain is utilized in various ways to make diagnoses. For example, a healthy brain exhibits a rough bilateral symmetry with respect to the interhemispheric fissure that bisects the brain. This fissure is commonly referred to as the anatomical mid-sagittal plane (MSP) and is shown in Fig. 1. The radiologists use the expected symmetry about the MSP to detect abnormalities. Because the head of the patient may be in an arbitrary position during scanning, the evaluation of hemispheric symmetry from the raw data is difficult.
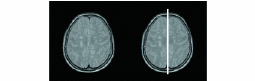
FIGURE 1 — The mid-sagittal plane location for the brain MR slice on the left is shown as a white line on the right.
Evaluation of high-resolution and mobile display systems for digital radiology in dark and bright environments using human and computational observers
Rebecca Vogel
Anindita Saha
Kish Chakrabarti
Aldo Badano
Food and Drug Administration
Abstract — As digital display systems replace film traditionally used for reading radiographic images, resource-intensive acceptance testing must be performed to ensure that quality meets and maintains desired specifications. If machine observers can replace human readers, whose performances are highly variable, the results will be more consistent and less costly. To be effective, however, the automated observers must track human performance. An approach for a model observer, validated with human readers, for the evaluation of the visibility of low-contrast small targets in high-resolution and mobile displays under different ambient illumination, will be described. The displays were tested using CDMAM-like digital phantoms containing disks of varying diameters and contrasts on a flat background. For this task, we find the best indicator of display performance to be the display's ability to represent small luminance contrast, not resolution or pixel size. The results confirm that high-resolution systems perform better under low illumination while illuminance has a minor impact on the mobile-display performance. Finally, the results show that the machine observer tracks the performance of human readers. Machine observers with proper validation can replace humans in the acceptance testing procedures, saving the testers both time and money.
Seven display systems were used in this study: four high-resolution monitors and three mobile displays. Of the four high-resolution displays, two were 5-Mpixel gray-scale monitors from different manufacturers, one was a 3-Mpixel color monitor, and one was a 1-Mpixel color monitor commercialized as medical-display monitors for use in radiology and other imaging fields such as reconnaissance, advanced graphics, and geospatial and military applications.
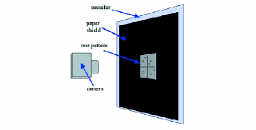
FIGURE 5 — The set-up of the acquisition of images for the machine observer.
Clinical applications for stereoscopic 3-D displays
David J. Getty
Patrick J. Green
BBN Technologies
Abstract — Stereoscopic 3-D digital imaging holds the promise of improving the detection, diagnosis, and treatment of disease as well as enhancing the training and preparation of medical professionals through use of stereoscopic 3-D displays in concert with the many volumetric visualization techniques/modalities developed in recent years. While so-called 3-D graphics have improved the state of computer visualization in general, 3-D displays make full use of the human-visual perception, and thus can provide critical insight in complex computer-generated and video 3-D data. The stereo 3-D applications reviewed in this paper include screening of breast cancer and diabetic retinopathy, visualization for minimally invasive surgery, and the teaching of anatomy. Also included is a discussion of groundbreaking results from a stereo digital mammography clinical trial under way at Emory University.
A clinical trial of stereoscopic digital mammography versus standard digital mammography in a screening setting is currently under way. The interim results from the trial are striking. In the current case sample, stereo mammography has reduced false-negative readings by 44% (27 false-negative readings by standard mammography, compared to only 15 by stereo mammography). Equally impressive, stereo mammography has reduced false-positive lesion detections in the current sample by 37% (68 false positive detections by standard mammography compared to only 43 for stereo mammography).

FIGURE 8 — Use of a 5-Mpixel Planar StereoMirror™ monitor in the Stereo Digital Mammography clinical trial.
Influence of 8-bit vs. 11-bit digital displays on observer performance and visual search: A multi-center evaluation
Elizabeth A. Krupinski
Khan Siddiqui
Eliot Siegel
Rasu Shrestha
Edward Grant
Hans Roehrig
Jiahua Fan
University of Arizona
Abstract — Medical-grade monochrome monitors typically display 8 bits of data. This study determined if 11-bit displays could improve observer performance and decrease use of window/level. 8- and 11-bit displays from three manufacturers were used at three sites. Six radiologists at each site viewed 100 DR chest images (half with a pulmonary nodule) on both displays. Decisions, confidence, nodule location, viewing time, and window/level use were recorded. There was no significant difference in ROC Az as a function of bit depth. The average Az with 8 bits was 0.8284 and with 11 bits was 0.8253. There was a significant difference in viewing time favoring the 11-bit displays. Window/level use did not differ. Eye position was recorded on a subset of images at one site. Cumulative dwell times for each decision category were lower with the 11-bit than with the 8-bit display. When tested with t-tests for paired observations, the TP (t =1.452, p = 0.1507), FN (t = 0.050, p = 0.9609), and FP (t = 0.042, p = 0.9676) were not statistically significant. The difference in the TN decisions was statistically significant (t = 1.926, p = 0.05). 8-bit displays will not impact negatively diagnostic accuracy, but using 11-bit displays may improve workflow efficiency.
Six observers at the site using the system C displays viewed the set of 20 images (15 with nodules, 5 without) as their eye position was recorded. Figure 4 shows a typical search pattern of one of the radiologists in the study. The circles represent fixations or locations where the eye lands with foveal (high resolution) vision. The size of the circle represents shorter (smaller) or longer (larger) dwell times. The lines connecting the circles represent saccades, or jumps, between the fixations and indicate the order in which the fixations were generated. The arrow in Fig. 4 indicates the location of the nodule. In this case, the radiologist fixated the nodule and reported it correctly (a true positive decision).
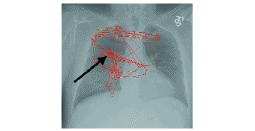
FIGURE 4 — Typical scanning pattern of a radiologist searching for pulmonary nodules. The arrow indicates the location of the nodule.
Computer-vision determination of 3-D geometric parameters of LDL particles via cryogenic transmission electron microscopy
W. Lewis Collier
Lenore M. Martin
Rik van Antwerpen
Capstone Visual Product Development
Abstract — Previous research has shown that the size of the LDL macromolecules can have an effect on cardiovascular health and that low-density lipoprotein (LDL) macromolecules may be non-spherical in shape. Some of these studies, however, used methods that are not conducive to automatic determination of the 3-D parameters of the particles. In particular, the prior methods used for determination of geometric-parameter determination were either centrifugal separations or manual determination of parameters from cryogenic transmission electron micrographs. An application of computer-vision techniques to automatically determine the 3-D parameters from cryogenic transmission electron microscopy (CTEM) images will be described. Correlation of computer-generated geometric models to the orthonormal projection CTEM imagery were investigated to determine the applicability of finding the pertinent geometric parameters of the expected discoid shape of the LDL particles. The processing showed that the discoid shape can be verified using small-angle rotations that are more amenable to the limitations of CTEM imaging.
The goal of this project was to retrieve 3-D parameters of height, width, and wall thickness from a minimum number of 2-D images. By requiring only a small number of images to reconstruct the biological artifact, the likelihood that the sample is distorted (i.e., melted or altered) by exposure to the electron beam is also significantly reduced.
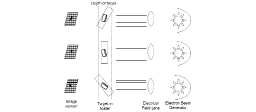
FIGURE 6 — CTEM ray paths and depth of focus.
|